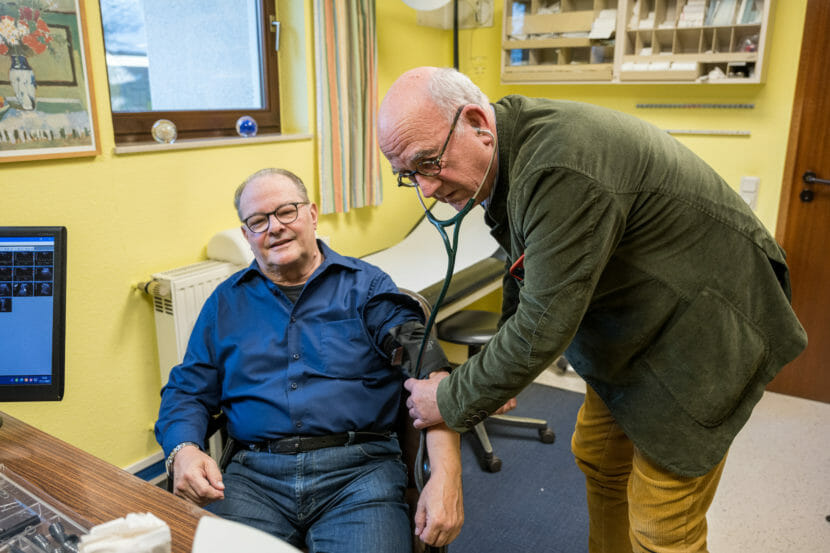
PÜTTLINGEN, Germany — Almost every day, Dr. Eckart Rolshoven sees the long shadow of coal mining in his clinic near the big brownstone church that dominates this small town in Germany’s Saarland.
The region’s last-operating coal shaft, just a few miles away, closed a decade ago, ending centuries of mining in the Saarland, a mostly rural state tucked between the Rhine River and the French border. But the mines left a difficult legacy, as they have in coal regions in the United States, including West Virginia.
Many of Rolshoven’s patients battle lung diseases and chronic pain from years of work underground. “We had an industry with a lot of illnesses,” said Rolshoven, a genial primary care physician who at 71 is nearing the end of a long career.
The Saarland’s residents are sicker than elsewhere in Germany. And like West Virginia, the region faces economic hurdles. For decades, German politicians, business leaders and unions have labored to adjust to the mining industry’s slow demise.
But this is a healthier place than West Virginia in many respects. The region’s residents are less likely to die prematurely, data shows. And on average, they live four years longer than West Virginians.
There is another important difference between this former coal territory and its Appalachian counterpart: West Virginia’s economic struggles have been compounded by medical debt, a burden that affects about 100 million people in the U.S. — in no state more than West Virginia.
In the Saarland, medical debt is practically nonexistent. It’s so rare in Germany that the federal government’s statistical office doesn’t even track it.
The reason isn’t government health care. Germany, like the U.S., has a largely private health care system that relies on private doctors and private insurers. Like Americans, many Germans enroll in a health plan through work, splitting the cost with their employer.
But Germany has long done something the U.S. does not: It strictly limits how much patients have to pay out of their own pockets for a trip to the doctor, the hospital or the pharmacy.
Rolshoven’s patients pay nothing when they see him. That not only bolsters their health, he said. It helps maintain what Rolshoven called social peace. “It’s really important not to have to worry about these problems,” he said.
German health officials, business leaders and economists say the access to affordable health care has also helped the Saarland get back on its feet economically, bolstered by the assurance that workers could get to the doctor.
“Without this, the Saarland would be dead,” said Beatrice Zeiger, managing director of the Arbeitskammer des Saarlandes, a regional labor group. “It’s unthinkable.”
While health costs rise in the U.S., Germany contains them
In West Virginia, whose wooded valleys and decaying industrial plants could be mistaken for the Saarland’s, access to health coverage has been important as the state weathered the decline of its mines.
A decade ago, state leaders moved to expand the Medicaid insurance program through the Affordable Care Act. And as of last year, just 6% of state residents were uninsured, less than half the rate before the 2010 law.
But growing numbers of West Virginians without government insurance are in private health plans with deductibles that require they pay thousands of dollars out of their own pockets before coverage kicks in.
The typical individual health plan an American gets through work now comes with a more than $1,500 deductible, a particularly big sum in a state like West Virginia where residents often earn less than residents of other states.
That, in turn, is driving medical debt. A quarter of West Virginians with a credit report have medical bills in collections, almost twice the national rate, according to data compiled by the nonprofit Urban Institute. In several counties in the state, the rate is about a third.
And those figures likely understate the problem. Many more people put medical bills on their credit cards, borrow from family or enroll in installment plans with a hospital or other providers to pay off their bills.
“It’s a huge problem here,” said Jessica Ice, executive director of West Virginians for Affordable Health Care. “Folks with medical debt aren’t able to apply for loans to start a business or buy a starter home for their family. It’s really preventing people from climbing up the economic ladder.”
In German health plans, known as sickness funds, there aren’t typically deductibles.
Physician visits are almost always free for patients. Copays for most prescription drugs are capped at 10 euros or less, about $10. And people admitted to the hospital pay only 10 euros a day.
“Access to medical care with minimal costs for patients has been essential,” said Armin Beck, regional director of the Knappschaft Bahn See, of KBS, a health insurance plan whose roots stretch back to the 13th century, when miners set up a mutual aid society to protect one another in case of injuries or accidents. “This has been a foundation of our community,” Beck said.
‘So glad we don’t have to worry’
Along the Saar River in Germany, rusting steelworks and shuttered coal-fired power plants bear testament to the region’s economic struggles. Many towns like Püttlingen carry on in the shadow of hulking mounds of debris — Berghalde, as they are called — the detritus left behind as coal was separated from the rocky earth hauled up from underground.

Today, new challenges confront the region. Ford, which has operated a car factory here for decades, plans to shutter the plant in a few years and move production to Spain.
But at Rolshoven’s clinic — a small set of offices tucked into a residential neighborhood — few patients can conceive of the burdens that medical bills put on Americans.
Andrea Fecht, 63, who has diabetes and came to see Rolshoven because recent tests revealed a concerning rise in her blood sugar, estimated she pays 120 euros a year, or about $125, to fill all six of her prescriptions, including her daily insulin.
In the U.S., the average price for insulin alone is nine times that in Germany, according to a recent report from Rand Corp., a research group.
Andreas Mang, a former miner who left the industry 20 years ago after a series of accidents, would likely pay even more out-of-pocket for his family’s drugs. Mang’s wife recently underwent a course of chemotherapy that would cost thousands of dollars if not for Germany’s limits on medical bills, Rolshoven said.
“I can’t imagine what it would be like not to have this support,” Mang said.
Christine Wagner said she’s had a glimpse of what Americans face. Wagner’s 18-year-old son, Jonas, has Down syndrome and has required more than 20 surgeries.
In global Facebook groups with other parents who have children with disabilities, Wagner said she’s amazed to see how much fundraising American parents do to pay family medical bills. “I’m so glad we don’t have to worry about that,” she said. “We have enough to do looking after Jonas.”
Countries where health care is actually affordable
International surveys underscore the difference Wagner observed between her experiences and those of American families.
In one recent study of health care in 11 high-income countries, the nonprofit Commonwealth Fund found that 44% of Americans had out-of-pocket medical expenses that topped $1,000 in the previous year. Just 16% of Germans reported paying that much. The rates were even lower in France, at 10%, and Great Britain, where only 7% reported similar medical expenses.
U.S. patients were also more than twice as likely as patients in any of the 10 other countries studied to say they had serious problems paying medical bills.
“Many Americans may not understand how affordable health care is for patients in other countries,” said Reginald D. Williams II, who oversees international research at the Commonwealth Fund. “Medical debt is a largely U.S. phenomenon. It just doesn’t happen in other countries.”
Most wealthy countries in Western Europe, East Asia and elsewhere limit patients’ out-of-pocket costs.
In the Netherlands, where patients enroll in private health plans as they do in Germany, insurers typically cover all medical expenses after patients pay a standard deductible of 385 euros, or about $400. Physician visits are fully covered.
In Great Britain, where medical care that is “free at the point of service” has been a foundation of that country’s government-run National Health Service for almost 75 years, there are rarely any doctor or hospital bills.
When the government asked Britons who’d gone into debt about the causes, just 2% cited paying for medical treatment. A similar share attributed their debt to gambling or another habit.
In the U.S., 41% of adults currently have debt from medical or dental bills, according to a KFF poll.
How Germany regulates hospital, doctor and drug prices
Germany’s strict limits on medical bills have periodically stoked concerns about patients overusing the health system.
But when health plans tried implementing a copay of 10 euros for physician visits, it was quickly rolled back amid criticism from patients and frustration among doctors, who didn’t like chasing after their patients for bills.

At the hospital in Püttlingen, which is operated by the Knappschaft, Dr. Marion Bolte said asking patients to pay more isn’t worth the risk, even if it might bring in more money.
“It’s better to have 20 unnecessary visits than to have one patient get harmed because they didn’t come to the hospital because they were worried about how much it would cost,” said Bolte, the chief medical officer. “We don’t want patients to worry about money. We want them to worry about getting better.”
Nationally, German patients are less likely than Americans to die from conditions that can be treated with good access to medical care, such as heart attacks, diabetes, pneumonia and some cancers, according to regional data compiled by the Paris-based Organization for Economic Cooperation and Development.
Germans are also less likely than Americans to say they had to wait to see a doctor, surveys show.
Lower-cost health care that protects workers from going into debt has meant fewer concerns for the Saarland’s policymakers, as well. “All that our predecessors had to worry about was creating jobs,” said Oliver Groll, a senior official at IHK Saarland, the regional chamber of commerce. “Health care took care of itself.”
As mining jobs disappeared, the Saarland shifted toward other industries, such as auto manufacturing, which has been a major employer since Ford opened its factory in 1970, sparking the development of a robust auto parts sector. The chamber and other business leaders are now working to lure technology and pharmaceutical jobs to the region.
For Mang, the former miner whose wife had cancer, knowing that medical bills wouldn’t drive him into debt helped give him the peace of mind to switch careers. “I never had to think about how much health care would cost me,” said Mang, who is now a nurse.
Maintaining this system has required that Germany do something else that U.S. policymakers have historically eschewed. Germany, like most wealthy nations, regulates the prices that hospitals, doctors and drugmakers can charge. This regulation occurs through a highly structured system in which insurers negotiate collectively with physician and hospital groups to set prices.
American hospitals and other medical providers for decades have fiercely resisted limits on their prices, spending millions to fight government regulation.
Price regulation can put more financial pressure on providers, who, unlike their American counterparts, can’t just demand higher prices from insurers to bolster their bottom lines.
Mario Schüller, the hospital administrator who runs the Knappschaft hospital in Püttlingen, said hospitals must instead compete to attract patients with better care and better customer service. Those that can’t compete may close, he said.
But Schüller said he wouldn’t want to charge patients more, even if he could.
“If I had to bill patients and then try to collect from them, I’d have to pay for all that,” he said. “We’d need new staff, who would have to get paid. And if we used collections companies, they’d have to be paid, too. It becomes a devil’s bargain.”
Copyright 2022 Kaiser Health News. To see more, visit Kaiser Health News.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.9(MDEwMjQ0ODM1MDEzNDk4MTEzNjU3NTRhYg004))


9(MDEwMjQ0ODM1MDEzNDk4MTEzNjU3NTRhYg004))


9(MDEwMjQ0ODM1MDEzNDk4MTEzNjU3NTRhYg004))



9(MDEwMjQ0ODM1MDEzNDk4MTEzNjU3NTRhYg004))