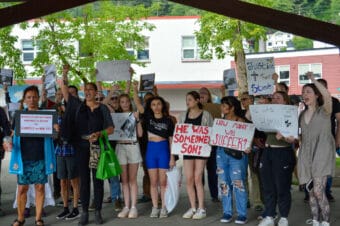Coast Guard officials call the rescue swimmer’s June 25 death “a tragedy,” urging comrades to use stress management resources on base.
Mental Health
Juneau’s hospital closes its crisis care unit less than a year after opening it
Bartlett Regional Hospital spokesperson Erin Hardin said the closure is due to a lack of funding and staff to keep the program afloat.
‘Devastated and angry’: Protestors call for change in the wake of deadly Juneau police shooting
The protesters gathered to express their anger over the death of Steven Kissack last week.
NAMI Juneau offers mental health resources to witnesses of downtown shooting
People who witnessed Monday’s deadly police shooting in downtown Juneau are carrying a lot of emotions — anger, confusion and grief, to name a few.
Alaska Senate considers plan that would allow teens to independently seek mental health care
An amendment from Sen. Cathy Giessel, R-Anchorage, would lower the age for obtaining behavioral health care to 16.
Psychologist sues state over license application she says is unconstitutional and discriminatory
Alaska is one of just a few states that screen for mental health history for a psychology license.